Looking for an Expert?
Yashoda Super Speciality MediCentre is home to some of
the eminent doctors in the world.
Yashoda Super Speciality Medicentre in Karkardooma, East Delhi, is designed to deliver world-class healthcare services, offering expert consultations, advanced diagnostics, and specialty services under one roof. Our centre is led by experienced doctors and supported by modern facilities to deliver advanced healthcare.
Our team of specialists offers expert consultations across a wide range of specialties

The Endocrinology Department at ...
Our fully equipped diagnostic wing provides accurate and timely investigations to support fast and effective treatment.
| ULTRASOUND | MON TO SAT | 10:00 AM TO 11:00 AM & 04:00 PM TO 05:00 PM |
| X-RAY / ECG | MON TO SAT | 09:00 AM TO 05:30 PM |
| Investigation (BLOOD Test) | MON TO SAT | 08:00 AM TO 4:30 PM |
| 2D - ECHO | MON & FRI | 03:00 AM TO 05:00 PM |

At our centre, we understand the emotional and physical challenges of infertility. Our dedicated IVF and Reproductive Medicine unit offers a complete range of fertility solutions tailored to your needs.

Success rates of up to 70–80% in women under 35, among the best in the region.
Expertise in advanced reproductive techniques, including ICSI, IMSI, blastocyst culture, and preimplantation genetic testing (PGT).

A team of highly experienced fertility specialists, embryologists, and counselors under one roof.

IVF Package Cost: ₹90,000/- + Injections
Other IVF Packages Cost:
Hormonal medications are administered to stimulate the ovaries to produce multiple eggs.
Progress is monitored through blood tests and ultrasound scans to track follicle growth and hormone levels.
Eggs are retrieved from the ovaries using a minimally invasive surgical procedure under anesthesia.
Sperm is collected from the male partner or a donor.
Eggs and sperm are combined in a laboratory dish for natural fertilization or via ICSI (Intracytoplasmic Sperm Injection).
Fertilized eggs develop into embryos over several days in the laboratory and are monitored for quality and development.
One or more embryos are transferred into the uterus using a thin catheter, guided by ultrasound, typically 3-5 days after fertilization.


Senior Consultant – Nephrology & Renal Transplant

Senior Consultant - Orthopedics with Joint Replace...

Senior Consultant - Nephrology & Renal Transplant

Sr. Consultant: Endocrinology and Metabolic diseas...

Head, Department of Physiotherapy

Senior Consultant Pediatrics

Senior Consultant Pediatrics

Senior Consultant – Internal Medicine

Senior consultant, Obstetrics and Gynaecologist

Consultant IVF and Infertility

Stay informed with the latest announcements, medical breakthroughs, and hospital highlights.
Recognized by leading newspapers and media outlets for our excellence in healthcare.




Robotic Milestone in Advanced Cancer Surgery: Combined Robotic LAR with Portal Vein Ligation
Our surgical oncology team recently achieved another important milestone in minimally invasive cancer surgery by successfully performing a Robotic Low Anterior Resection (LAR) combined with robotic ligation of the right portal vein in a 50-year-old female diagnosed with rectal cancer and synchronous liver metastasis.
The patient presented with rectal adenocarcinoma along with metastatic disease involving the right lobe of the liver. Managing such complex cases requires meticulous planning to achieve complete o...
Robotic Milestone in Advanced Cancer Surgery: Combined Robotic LAR with Portal Vein Ligation
Our surgical oncology team recently achieved another important milestone in minimally invasive cancer surgery by successfully performing a Robotic Low Anterior Resection (LAR) combined with robotic ligation of the right portal vein in a 50-year-old female diagnosed with rectal cancer and synchronous liver metastasis.
The patient presented with rectal adenocarcinoma along with metastatic disease involving the right lobe of the liver. Managing such complex cases requires meticulous planning to achieve complete oncological clearance while preserving adequate liver function.
After multidisciplinary tumor board discussion, a staged surgical strategy was planned with curative intent. In the first stage, a robotic low anterior resection was performed following total mesorectal excision principles to remove the rectal primary tumor. During the same sitting, robotic ligation of the right branch of the portal vein was carried out. This step is designed to induce hypertrophy of the future liver remnant, allowing safe completion of a planned right hepatectomy after approximately four weeks.
The use of robotic technology enabled precise pelvic dissection, superior visualization, and delicate hilar vascular control, allowing two major oncologic objectives to be achieved through a minimally invasive approach. The patient tolerated the procedure well and is recovering satisfactorily while awaiting the second-stage liver surgery.
This combined robotic approach highlights the evolving role of advanced minimally invasive surgery in complex gastrointestinal and hepatobiliary oncology. By integrating colorectal and liver strategies in a single operation, patients benefit from reduced surgical trauma, faster recovery, and preservation of curative treatment pathways.
The case reflects our institution’s continued commitment to innovation, multidisciplinary collaboration, and delivery of world-class cancer care using cutting-edge robotic surgical techniques.
Treatment By:
Dr. Asim Rizvi

A professional WWE wrestler sustained a knee injury during a wrestling bout while on tour in India, resulting in acute pain, instability, and inability to continue performance. Clinical and radiological evaluation confirmed an anterior cruciate ligament (ACL) tear along with a concomitant meniscus injury.
He was evaluated by the orthopaedic team, led by Dr. Brajesh Koushle, and was advised to undergo surgical intervention to restore knee stability and enable early return to high-impact activity. Given the functional demands of a professional athlete, a minimally invasive, precision-driven approach was planned.
The pat...
A professional WWE wrestler sustained a knee injury during a wrestling bout while on tour in India, resulting in acute pain, instability, and inability to continue performance. Clinical and radiological evaluation confirmed an anterior cruciate ligament (ACL) tear along with a concomitant meniscus injury.
He was evaluated by the orthopaedic team, led by Dr. Brajesh Koushle, and was advised to undergo surgical intervention to restore knee stability and enable early return to high-impact activity. Given the functional demands of a professional athlete, a minimally invasive, precision-driven approach was planned.
The patient underwent arthroscopic ACL reconstruction using an advanced Xiros ligament system, along with an all-inside meniscus repair. The procedure was performed using keyhole techniques, ensuring minimal tissue disruption and optimal anatomical restoration.
Postoperatively, the patient showed rapid recovery. Early mobilisation was initiated, and he was able to bear weight and walk on both limbs from the very next day. With structured rehabilitation, he is on track for a timely return to professional wrestling within a few weeks.
Treatment By:
Dr. Brajesh Koushle and Team

A 71-year-old female from Kazakhstan presented with persistent hip pain and a limp, significantly affecting her mobility and quality of life. She had a history of prior fracture fixation surgery of the left hip, which had failed over time, leading to joint deterioration, chronic pain, and functional limitation.
On clinical and radiological evaluation, the left hip joint was found to be severely compromised due to failed implant fixation. She was assessed by the orthopaedic team, who recommended revision hip arthroplasty as the definitive treatment, given the extent of joint damage and prolonged disability.
The patient...
A 71-year-old female from Kazakhstan presented with persistent hip pain and a limp, significantly affecting her mobility and quality of life. She had a history of prior fracture fixation surgery of the left hip, which had failed over time, leading to joint deterioration, chronic pain, and functional limitation.
On clinical and radiological evaluation, the left hip joint was found to be severely compromised due to failed implant fixation. She was assessed by the orthopaedic team, who recommended revision hip arthroplasty as the definitive treatment, given the extent of joint damage and prolonged disability.
The patient underwent a complex revision procedure involving the removal of the existing implant with careful preservation of bone stock, followed by a revision total hip replacement. The surgery required meticulous planning and execution due to altered anatomy and previous surgical intervention.
Postoperatively, the patient demonstrated excellent recovery. Early mobilisation was initiated, and she was able to take her first steps the following day with a stable, pain-free gait. After nearly two decades of impaired mobility, she achieved independent ambulation without a limp and was discharged in stable condition.
Treatment By:
Dr. Brajesh Koushle, Dr. Gaurav Thakral, and Team

A 59-year-old female from Comoros presented with severe bilateral knee dysfunction and associated implant-related complications. She had a Grade 3 valgus deformity with advanced osteoarthritis, a failed primary total knee replacement of the left knee, and significant implant impingement at the left ankle, resulting in marked pain and restricted mobility.
She was evaluated by the orthopaedic team at Yashoda Medicity led by Dr. Brajesh Koushle and Dr. Gaurav Thakral, at Yashoda Medicity. Given the complexity of her condition and functional limitations, a comprehensive surgical plan was formulated.
The patient unde...
A 59-year-old female from Comoros presented with severe bilateral knee dysfunction and associated implant-related complications. She had a Grade 3 valgus deformity with advanced osteoarthritis, a failed primary total knee replacement of the left knee, and significant implant impingement at the left ankle, resulting in marked pain and restricted mobility.
She was evaluated by the orthopaedic team at Yashoda Medicity led by Dr. Brajesh Koushle and Dr. Gaurav Thakral, at Yashoda Medicity. Given the complexity of her condition and functional limitations, a comprehensive surgical plan was formulated.
The patient underwent primary total knee replacement of the right knee, revision total knee replacement of the left knee, and removal of the impinging implant from the left ankle in the same sitting. The surgery was successfully completed with meticulous intraoperative management.
Postoperatively, the patient showed excellent recovery. Early mobilisation was initiated, and she was able to stand and walk from the first post-operative day. She was discharged in a stable condition, walking unassisted and with significant improvement in functional outcomes.
Treatment By:
Dr. Brajesh Koushle, Dr. Gaurav Thakral, and Team

A 65-year-old female, a known carcinoma colon survivor, presented with altered sensorium, severe headache, diplopia, and worsening vision.
On arrival, she was drowsy, disoriented, with gaze palsy, hemianopia, and significantly elevated blood pressure. MRI brain revealed a large left occipital tumor with acute haemorrhage, requiring emergency intervention.
She underwent urgent craniotomy with total tumor excision and evacuation of the hematoma. The surgery was completed successfully.
Post-operatively, she showed rapid and remarkable recovery, with significant improvement in neurological status. She was discharge...
A 65-year-old female, a known carcinoma colon survivor, presented with altered sensorium, severe headache, diplopia, and worsening vision.
On arrival, she was drowsy, disoriented, with gaze palsy, hemianopia, and significantly elevated blood pressure. MRI brain revealed a large left occipital tumor with acute haemorrhage, requiring emergency intervention.
She underwent urgent craniotomy with total tumor excision and evacuation of the hematoma. The surgery was completed successfully.
Post-operatively, she showed rapid and remarkable recovery, with significant improvement in neurological status. She was discharged in four days and, at one-week follow-up, was walking independently with restored clarity of vision and no headache.
Her recovery was exceptional for the extent of pathology and age, with neurological improvement far exceeding expected timelines.
Treatment By:
Dr. Rajinder Kumar

Minimally invasive and Scarless solution for Brain aneurysm at Yashoda Medicity
A patient with a complex brain aneurysm was treated at Yashoda Medicity through a minimally invasive and scarless approach. This was the first neurointervention for a complex brain aneurysm in the state, performed in our state-of-the-art Philips Biplanar Cath Lab, equipped with advanced softwares including 3D angiography, CBCT, Xper CT, VasoCT, MAFA, and Clarity IQ.
The procedure was led by Dr. Dibya Jyoti Mahakul, Consultant – Endovascular Neurosurgery, who carefully placed a Flow Diverter Stent across the aneurysm. Us...
Minimally invasive and Scarless solution for Brain aneurysm at Yashoda Medicity
A patient with a complex brain aneurysm was treated at Yashoda Medicity through a minimally invasive and scarless approach. This was the first neurointervention for a complex brain aneurysm in the state, performed in our state-of-the-art Philips Biplanar Cath Lab, equipped with advanced softwares including 3D angiography, CBCT, Xper CT, VasoCT, MAFA, and Clarity IQ.
The procedure was led by Dr. Dibya Jyoti Mahakul, Consultant – Endovascular Neurosurgery, who carefully placed a Flow Diverter Stent across the aneurysm. Using MAFA software, the first of its kind in North India, the team successfully achieved and recorded the target aneurysmal flow parameters.
The use of these advanced technologies aided in faster decision-making, reduced radiation exposure, and improved procedural precision, reflecting our belief that “Time is Brain.” This case demonstrates our preparedness to manage all varieties of complex neurovascular conditions, from ischemic stroke to hemorrhagic stroke, through minimally invasive and scarless procedures.
When it comes to neurointervention and endovascular neurosurgery, Yashoda Medicity, equipped with the latest technologies and expert teams, is miles ahead in delivering advanced patient care.
Treatment By:
Dr. Dibya Jyoti Mahakul

Advanced otology and cochlear implant surgery play a critical role in restoring hearing in patients with severe to profound hearing loss. At Yashoda Medicity, Mr. Raghav, a 45-year-old male, developed progressive hearing impairment following a road traffic accident a year ago, during which he sustained multiple injuries and underwent repeated surgeries. Over time, he experienced worsening bilateral hearing loss, with limited benefit from hearing aids. Evaluation suggested ototoxicity as the likely cause, resulting in irreversible inner ear damage.
After detailed assessment, cochlear implant surgery was performed for his wor...
Advanced otology and cochlear implant surgery play a critical role in restoring hearing in patients with severe to profound hearing loss. At Yashoda Medicity, Mr. Raghav, a 45-year-old male, developed progressive hearing impairment following a road traffic accident a year ago, during which he sustained multiple injuries and underwent repeated surgeries. Over time, he experienced worsening bilateral hearing loss, with limited benefit from hearing aids. Evaluation suggested ototoxicity as the likely cause, resulting in irreversible inner ear damage.
After detailed assessment, cochlear implant surgery was performed for his worse ear. The procedure was completed successfully, and the patient was discharged the next day in stable condition. The device was activated on the fifth postoperative day, following which he showed significant improvement in hearing and communication.
He is now able to interact comfortably with his family and participate in conversations, reflecting a marked improvement in quality of life.
Treatment By:
Dr Shashank Vashist.

Advanced minimally invasive surgery plays a critical role in managing complex abdominal conditions, enabling precise intervention with faster recovery and reduced surgical impact. At the Yashoda Institute of Minimal Access, Robotic and Bariatric Surgery (MARBS), a 38-year-old male presented with low-grade adenocarcinoma of the colon, with mucosal extension and partial luminal obstruction.
Following preoperative optimisation in coordination with the Gastroenterology team, the patient underwent a laparoscopically assisted left limited hemicolectomy with partial mesocolon excision.
The colocolic anastomosis was completed...
Advanced minimally invasive surgery plays a critical role in managing complex abdominal conditions, enabling precise intervention with faster recovery and reduced surgical impact. At the Yashoda Institute of Minimal Access, Robotic and Bariatric Surgery (MARBS), a 38-year-old male presented with low-grade adenocarcinoma of the colon, with mucosal extension and partial luminal obstruction.
Following preoperative optimisation in coordination with the Gastroenterology team, the patient underwent a laparoscopically assisted left limited hemicolectomy with partial mesocolon excision.
The colocolic anastomosis was completed through a small 2-inch subcostal incision, maintaining a minimally invasive approach while ensuring surgical precision. The postoperative course was uneventful, and the patient was discharged in a stable condition on Day 5.
This case reflects the strength of a minimally invasive surgical approach in managing complex cases, enabling effective treatment with faster recovery and improved patient outcomes.
Treatment By:
Dr. P.K. Dewan, Dr. Abhimanyu Dewan, Dr. Ismail Khan, and Dr. Pooja

Advanced minimally invasive surgery plays a critical role in managing complex surgical cases that are often considered high-risk. At the Yashoda Institute of Minimal Access, Robotic and Bariatric Surgery (MARBS), a 45-year-old male presented with severe epigastric pain and was diagnosed with acute calculous cholecystitis. He had previously consulted multiple surgeons for a routine laparoscopic cholecystectomy but was declined due to a large laparotomy scar from a prior splenectomy and the presence of portal hypertension.
After careful evaluation, a completely laparoscopic approach was planned despite the surgical challeng...
Advanced minimally invasive surgery plays a critical role in managing complex surgical cases that are often considered high-risk. At the Yashoda Institute of Minimal Access, Robotic and Bariatric Surgery (MARBS), a 45-year-old male presented with severe epigastric pain and was diagnosed with acute calculous cholecystitis. He had previously consulted multiple surgeons for a routine laparoscopic cholecystectomy but was declined due to a large laparotomy scar from a prior splenectomy and the presence of portal hypertension.
After careful evaluation, a completely laparoscopic approach was planned despite the surgical challenges. The procedure was performed with precision, successfully navigating the complexities associated with prior surgery and altered anatomy.
The surgery was completed successfully, and the patient had an excellent postoperative recovery. He was discharged in a stable condition on Day 2 following the procedure.
This case was led by Dr. P.K. Dewan, along with Dr. Abhimanyu Dewan, Dr. Ismail Khan, and Dr. Pooja, supported by the experienced surgical and nursing teams.
It reflects the strength of advanced laparoscopic expertise in safely managing complex and previously declined cases, enabling effective treatment with faster recovery and improved patient outcomes.
Treatment By:
Dr. P.K. Dewan, Dr. Abhimanyu Dewan, Dr. Ismail Khan, and Dr. Pooja

Advanced minimally invasive surgery plays a critical role in managing complex cases with high surgical risk, offering safer outcomes and faster recovery. In a recent breakthrough case at the Yashoda Institute of Minimal Access, Robotic and Bariatric Surgery (MARBS), a 73-year-old patient with chronic liver disease and portal hypertension, along with diabetes, hypertension, and severe anemia due to hypersplenism, was successfully treated. The patient had been dependent on repeated blood transfusions, with increasing frequency over the past two years.
After a detailed clinical evaluation, a laparoscopically assisted splenec...
Advanced minimally invasive surgery plays a critical role in managing complex cases with high surgical risk, offering safer outcomes and faster recovery. In a recent breakthrough case at the Yashoda Institute of Minimal Access, Robotic and Bariatric Surgery (MARBS), a 73-year-old patient with chronic liver disease and portal hypertension, along with diabetes, hypertension, and severe anemia due to hypersplenism, was successfully treated. The patient had been dependent on repeated blood transfusions, with increasing frequency over the past two years.
After a detailed clinical evaluation, a laparoscopically assisted splenectomy was planned as a definitive treatment. The procedure was performed using a minimally invasive approach, enabling precise removal of the enlarged spleen while minimising surgical stress in a high-risk patient.
The surgery was completed successfully, and the patient had an uneventful postoperative recovery. Following the procedure, the need for repeated blood transfusions was effectively resolved, marking a significant improvement in the patient’s clinical condition.
This case was led by Dr. P.K. Dewan, along with Dr. Abhimanyu Dewan, Dr. Ismail Khan, and Dr. Pooja, supported by the experienced surgical and nursing teams.
It reflects the strength of advanced laparoscopic techniques in managing complex conditions, offering definitive treatment while reducing complications and supporting improved quality of life for patients.
Treatment By:
Dr. P.K. Dewan, Dr. Abhimanyu Dewan, Dr. Ismail Khan, and Dr. Pooja

Advanced endoscopic care plays a critical role in managing complex pancreatic conditions, offering effective non-surgical alternatives with reduced risk and faster recovery. In a recent case, our team successfully treated a 68-year-old male with a history of pancreatitis, who presented with severe upper abdominal pain, signs of infection, gastric outlet narrowing, and jaundice. He was found to have a large pancreatic walled-off necrosis measuring 8 × 9 cm on admission.
A structured, stepwise approach was followed. On Day 1, imaging, including CECT abdomen and endoscopic ultrasound, was performed to assess the extent of t...
Advanced endoscopic care plays a critical role in managing complex pancreatic conditions, offering effective non-surgical alternatives with reduced risk and faster recovery. In a recent case, our team successfully treated a 68-year-old male with a history of pancreatitis, who presented with severe upper abdominal pain, signs of infection, gastric outlet narrowing, and jaundice. He was found to have a large pancreatic walled-off necrosis measuring 8 × 9 cm on admission.
A structured, stepwise approach was followed. On Day 1, imaging, including CECT abdomen and endoscopic ultrasound, was performed to assess the extent of the collection. On Day 2, a lumen-apposing metal stent (LAMS) was placed through the gastric lumen into the pancreatic collection, allowing significant internal drainage.
On Day 5, the team accessed the collection through the same route and removed the damaged tissue, followed by reassessment and further clearance on Day 8 to ensure healthy healing. The stent was managed in stages, with removal of the metallic stent and replacement with a plastic stent on Day 25 to support recovery.
By Day 40, the patient had completely recovered and continues to remain stable on follow-up.
This case reflects the strength of a minimally invasive, stepwise approach in treating complex pancreatic necrosis. It avoids major surgery while ensuring effective recovery and improved patient outcomes.
Treatment By:
Dr. Rajesh Upadhyay, Dr. V. S. Gaurav Narayan, and Dr. Priyanka Ramnivas Ojha

A 27-year-old patient diagnosed with advanced-stage T-cell lymphoma presented for specialised evaluation and management. Given the aggressive nature of the disease, a detailed clinical assessment and a structured treatment plan were undertaken by the expert team.
The patient was treated with high-dose chemotherapy followed by an autologous stem cell transplant, a well-established approach for managing advanced hematological malignancies. The treatment was carried out under the expertise of Dr. Nivedita Dhingra, Director & Head – Hematology, Hemato-Oncology and Bone Marrow Transplant (Adult & Pediatrics), along wit...
A 27-year-old patient diagnosed with advanced-stage T-cell lymphoma presented for specialised evaluation and management. Given the aggressive nature of the disease, a detailed clinical assessment and a structured treatment plan were undertaken by the expert team.
The patient was treated with high-dose chemotherapy followed by an autologous stem cell transplant, a well-established approach for managing advanced hematological malignancies. The treatment was carried out under the expertise of Dr. Nivedita Dhingra, Director & Head – Hematology, Hemato-Oncology and Bone Marrow Transplant (Adult & Pediatrics), along with Dr. Karuna Jha, Senior Consultant – Hematology, Hemato-Oncology and Bone Marrow Transplant (Adult & Pediatrics), supported by the dedicated BMT team.
The treatment protocol was designed to achieve optimal disease control while ensuring patient safety. High-dose chemotherapy helped target and eliminate malignant cells, followed by stem cell reinfusion to restore healthy bone marrow function.
The patient responded well to the treatment and was closely monitored throughout the recovery phase, demonstrating a stable clinical course post-procedure.
This case highlights the importance of a protocol-based, multidisciplinary approach in managing rare and complex lymphomas, combining clinical expertise with advanced transplant capabilities to achieve effective outcomes.
Treatment By:
Dr. Nivedita Dhingra & Dr. Karuna Jha

Advanced neonatal care plays a critical role in improving survival and long-term outcomes for extremely preterm infants. In a recent case, our multidisciplinary team successfully managed the delivery and care of a baby boy born at just 26 weeks of gestation, weighing under 800 grams.
The newborn required immediate respiratory support and was admitted to a Level III Neonatal Intensive Care Unit (NICU), where he received round-the-clock monitoring and specialised care. Through meticulous medical management and dedicated nursing support, the baby demonstrated consistent progress over the course of treatment.
He was disch...
Advanced neonatal care plays a critical role in improving survival and long-term outcomes for extremely preterm infants. In a recent case, our multidisciplinary team successfully managed the delivery and care of a baby boy born at just 26 weeks of gestation, weighing under 800 grams.
The newborn required immediate respiratory support and was admitted to a Level III Neonatal Intensive Care Unit (NICU), where he received round-the-clock monitoring and specialised care. Through meticulous medical management and dedicated nursing support, the baby demonstrated consistent progress over the course of treatment.
He was discharged in a stable condition, breathing independently and feeding well, marking a significant milestone in his recovery journey.
This case was led by Dr. Neha Agrawal, Consultant – Pediatrics & Neonatology; Dr. J.B. Sharma, Principal Director & Head – Obstetrics and Gynaecology; Dr. Namita Nigam Datta, Senior Consultant – Obstetrics and Gynaecology; and Dr. Nisha, Consultant – Obstetrics & Gynaecology, alongside our experienced nursing and clinical teams.
It reflects the strength of coordinated clinical expertise, advanced neonatal infrastructure, and a commitment to delivering specialised care focused on giving every newborn the best possible start in life.
Treatment By:
Dr. Neha Agrawal, Dr. J.B. Sharma, Dr. Namita Nigam Datta, Dr. Nisha

A patient diagnosed with a tumour in the head of the pancreas presented for specialised evaluation and management. Given the complexity of the condition, a detailed clinical assessment and surgical planning were undertaken by the expert team.
The patient was planned for a Robotic Pancreaticoduodenectomy (Whipple’s Procedure), a highly specialised surgery used to treat tumours in this region. The procedure was performed under the expertise of Dr. Syed Asim Rizvi, Principal Director – Surgical Oncology and Robotic Surgery, along with his team, using advanced robotic surgical technology.
The robotic approach provided...
A patient diagnosed with a tumour in the head of the pancreas presented for specialised evaluation and management. Given the complexity of the condition, a detailed clinical assessment and surgical planning were undertaken by the expert team.
The patient was planned for a Robotic Pancreaticoduodenectomy (Whipple’s Procedure), a highly specialised surgery used to treat tumours in this region. The procedure was performed under the expertise of Dr. Syed Asim Rizvi, Principal Director – Surgical Oncology and Robotic Surgery, along with his team, using advanced robotic surgical technology.
The robotic approach provided enhanced precision and superior visualisation, enabling meticulous removal of the tumour while preserving surrounding structures. This minimally invasive technique also helped reduce intraoperative blood loss and supported a more controlled surgical environment.
The patient demonstrated a smooth postoperative recovery with reduced pain, early mobilisation, and overall improved comfort. He was discharged in stable condition.
This case highlights the role of advanced robotic surgery in managing complex pancreatic tumours, combining surgical expertise with precision technology to achieve optimal patient outcomes.
Treatment By:
Dr. Asim Rizvi

A 39-year-old patient from Nairobi presented with symptoms of obstructive jaundice and required urgent evaluation. A comprehensive diagnostic workup, including advanced imaging and endoscopic assessment, confirmed the diagnosis of pancreatic cancer.
The clinical team first focused on stabilising the patient and relieving the obstruction. A therapeutic endoscopic procedure with stenting was performed, leading to improvement in symptoms and liver function. Once optimised, the patient was carefully planned for definitive surgical management.
The surgery was performed under the expertise of Dr. Syed Asim Rizvi, Principal ...
A 39-year-old patient from Nairobi presented with symptoms of obstructive jaundice and required urgent evaluation. A comprehensive diagnostic workup, including advanced imaging and endoscopic assessment, confirmed the diagnosis of pancreatic cancer.
The clinical team first focused on stabilising the patient and relieving the obstruction. A therapeutic endoscopic procedure with stenting was performed, leading to improvement in symptoms and liver function. Once optimised, the patient was carefully planned for definitive surgical management.
The surgery was performed under the expertise of Dr. Syed Asim Rizvi, Principal Director – Surgical Oncology and Robotic Surgery, using advanced robotic surgical technology. This approach enabled enhanced precision, minimal blood loss, and a minimally invasive pathway to treatment.
The patient showed a smooth postoperative recovery, with early initiation of oral intake, timely mobilisation, and reduced discomfort. He was discharged in stable condition within a week of the procedure.
This case highlights the importance of timely diagnosis, structured clinical management, and the role of advanced robotic surgery in improving outcomes for complex pancreatic cancer cases.
Treatment By:
Dr. Asim Rizvi

A patient with a long-standing history of lymphedema in her right arm since 2014 presented with persistent swelling and concerning changes in the affected limb. Clinical evaluation and further investigations, including PET scan and FNAC, confirmed the presence of a rare and aggressive malignancy involving the cutaneous and subcutaneous tissues of the forearm, diagnosed as lymphangiosarcoma.
Given the complexity of the condition and the risk to limb function, a carefully planned, patient-centric treatment approach was undertaken under the care of Dr. Manish Singhal, Vice Chairman – Medical Oncology, Yashoda Institute of Ca...
A patient with a long-standing history of lymphedema in her right arm since 2014 presented with persistent swelling and concerning changes in the affected limb. Clinical evaluation and further investigations, including PET scan and FNAC, confirmed the presence of a rare and aggressive malignancy involving the cutaneous and subcutaneous tissues of the forearm, diagnosed as lymphangiosarcoma.
Given the complexity of the condition and the risk to limb function, a carefully planned, patient-centric treatment approach was undertaken under the care of Dr. Manish Singhal, Vice Chairman – Medical Oncology, Yashoda Institute of Cancer Care.
The patient was treated with a combination of advanced chemotherapy and targeted therapy. The treatment was precisely tailored to control disease progression while prioritising limb preservation.
She responded well to therapy, with effective disease control achieved without the need for amputation. The limb was successfully preserved, maintaining both function and quality of life.
This case highlights the role of precision oncology and timely intervention in managing rare and challenging cancers, demonstrating how advanced treatment strategies can achieve optimal outcomes while preserving function and improving patient well-being.
Treatment By:
Dr. Manish Singhal

A 78-year-old male patient presented with difficulty in swallowing and a small growth at the base of the tongue. Initial evaluation, including biopsy and imaging, confirmed a malignancy involving the tongue along with an affected lymph node in the neck.
As part of routine staging, a whole-body scan revealed an additional lesion in the upper lobe of the lung with associated chest lymph nodes. Further evaluation confirmed this to be a second, unrelated primary cancer. This rare presentation of two simultaneous primary cancers required a carefully coordinated and highly specialised treatment approach.
After a detailed as...
A 78-year-old male patient presented with difficulty in swallowing and a small growth at the base of the tongue. Initial evaluation, including biopsy and imaging, confirmed a malignancy involving the tongue along with an affected lymph node in the neck.
As part of routine staging, a whole-body scan revealed an additional lesion in the upper lobe of the lung with associated chest lymph nodes. Further evaluation confirmed this to be a second, unrelated primary cancer. This rare presentation of two simultaneous primary cancers required a carefully coordinated and highly specialised treatment approach.
After a detailed assessment by a multidisciplinary team, a comprehensive treatment plan was developed with curative intent. The patient was treated using advanced adaptive radiotherapy, a technique that allows real-time adjustments to radiation delivery based on daily imaging and anatomical changes, ensuring high precision and safety.
Both cancers were treated concurrently. The lung and chest lymph nodes received a planned course of radiation over six weeks, while the tongue and neck region were treated over seven weeks. Each session was guided by high-resolution imaging, enabling accurate targeting of the tumours while preserving surrounding healthy structures. The patient completed the treatment successfully with good tolerance. He showed a steady recovery and continues to remain stable on follow-up.
This case highlights the power of advanced radiation technology and multidisciplinary expertise in managing rare and complex cancer presentations.
Treatment By:
Dr. Gagan Saini

A 55-year-old woman diagnosed with advanced high-grade serous ovarian cancer presented after completing three cycles of neoadjuvant chemotherapy. She had responded well to treatment, with imaging showing significant disease resolution and tumour markers returning to normal levels. Following a comprehensive evaluation, she was planned for interval debulking surgery combined with Heated Intraperitoneal Chemotherapy (HIPEC).
After detailed counselling and preoperative optimisation, the patient underwent surgery under the care of the expert team. A meticulous cytoreductive procedure was performed to remove all visible disease, ...
A 55-year-old woman diagnosed with advanced high-grade serous ovarian cancer presented after completing three cycles of neoadjuvant chemotherapy. She had responded well to treatment, with imaging showing significant disease resolution and tumour markers returning to normal levels. Following a comprehensive evaluation, she was planned for interval debulking surgery combined with Heated Intraperitoneal Chemotherapy (HIPEC).
After detailed counselling and preoperative optimisation, the patient underwent surgery under the care of the expert team. A meticulous cytoreductive procedure was performed to remove all visible disease, followed by the administration of HIPEC, a targeted chemotherapy delivered directly into the abdominal cavity using specialised equipment over a controlled duration. The entire procedure was carried out with precise monitoring and a highly coordinated approach.
Postoperatively, the patient was closely monitored with a structured care protocol, including optimal fluid management and regular assessment of clinical parameters to support recovery.
The patient demonstrated a smooth and steady recovery and was discharged in stable condition on the eighth postoperative day. She continues to do well on follow-up.
This case marks a significant milestone as one of the successful HIPEC procedures performed at Yashoda Medicity, highlighting the team’s expertise in delivering advanced oncological care with precision and safety.
Treatment By:
Dr. Satinder Kaur, Dr. Hemlata Garg, and Dr. Ipshita Sahoo

A 30-year-old woman presented with abdominal fullness and on/off pain for the last 3 months, without any menstrual concerns. Imaging revealed a large abdomino-pelvic mass with multiple nodular growths extending into the abdomen, suggestive of a rare condition where multiple fibroids are spread across the abdominal cavity and involve surrounding organs.
After detailed evaluation and counselling, a surgical plan was carefully designed with a strong focus on preserving her fertility. The patient underwent exploratory surgery under the care of the expert team.
During the procedure, multiple fibroids of varying sizes were...
A 30-year-old woman presented with abdominal fullness and on/off pain for the last 3 months, without any menstrual concerns. Imaging revealed a large abdomino-pelvic mass with multiple nodular growths extending into the abdomen, suggestive of a rare condition where multiple fibroids are spread across the abdominal cavity and involve surrounding organs.
After detailed evaluation and counselling, a surgical plan was carefully designed with a strong focus on preserving her fertility. The patient underwent exploratory surgery under the care of the expert team.
During the procedure, multiple fibroids of varying sizes were identified arising from the uterus and extending into the pelvic and upper abdominal regions. A highly precise and carefully controlled surgical approach was adopted to safely remove the fibroids while preserving the uterus and both ovaries.
The surgery lasted approximately five hours, during which 15 fibroids weighing nearly 3 kg were successfully removed with minimal blood loss. The uterus and both ovaries were preserved, maintaining the patient’s reproductive potential.
The patient had a smooth recovery and was discharged in stable condition. This case highlights the team’s expertise in managing rare and complex conditions with a focus on precision, safety, and organ preservation, ensuring the best possible outcome for the patient.
Treatment By:
Dr. Satinder Kaur, Dr. Hemlata Garg, and Dr. Ipshita Sahoo

A 65-year-old male patient, weighing 44 kg, presented with long-standing coronary artery disease, a recent myocardial infarction, critical multivessel disease, unstable angina, and severe left ventricular dysfunction with a left ventricular ejection fraction (LVEF) of 20–25%. Considering the complexity of his condition, he underwent coronary artery bypass grafting (CABG) under the care of the expert cardiac team.
The procedure was successfully performed, with the patient requiring minimal inotropic support and no intra-aortic balloon pump (IABP). He was extubated within four hours, reflecting a stable and well-managed imm...
A 65-year-old male patient, weighing 44 kg, presented with long-standing coronary artery disease, a recent myocardial infarction, critical multivessel disease, unstable angina, and severe left ventricular dysfunction with a left ventricular ejection fraction (LVEF) of 20–25%. Considering the complexity of his condition, he underwent coronary artery bypass grafting (CABG) under the care of the expert cardiac team.
The procedure was successfully performed, with the patient requiring minimal inotropic support and no intra-aortic balloon pump (IABP). He was extubated within four hours, reflecting a stable and well-managed immediate postoperative course.
Post-surgery, the patient was closely monitored and managed with a highly calibrated clinical approach. Advanced hemodynamic support strategies, including the timely use of an intra-aortic balloon pump (IABP), along with optimised inotropic management, judicious fluid administration, and targeted medical therapy, ensured effective systemic and organ perfusion.
Over the next few days, the patient demonstrated steady clinical improvement, with stabilising metabolic parameters, improving organ function, and gradual return to normal physiological activity. This enabled the phased withdrawal of advanced support measures, including ventilatory and circulatory assistance.
Following a structured period of intensive care and rehabilitation, the patient was discharged in stable condition. The case highlights the team’s expertise in managing complex high-risk cardiac conditions with precision, resulting in a successful recovery.
Treatment By:
Dr. Rachit Saxena, Dr. Vikas Kumar Keshari, and Dr. Kushant Gupta

Timely Care at Yashoda Medicity Helps International Patient Recover from Serious Lung Infection
A patient from Kazakhstan developed a serious lung infection after undergoing medical treatment that weakened his immunity. Despite receiving treatment multiple times in his home country, his condition did not improve, prompting his family to seek further care in India.
A detailed chest scan revealed a large infected area in the lung, suggesting a long-standing problem. The procedure to closely evaluate the lungs was performed at the Yashoda Institute of Respiratory Medicine and Interventional Pulmonology, under the care of...
Timely Care at Yashoda Medicity Helps International Patient Recover from Serious Lung Infection
A patient from Kazakhstan developed a serious lung infection after undergoing medical treatment that weakened his immunity. Despite receiving treatment multiple times in his home country, his condition did not improve, prompting his family to seek further care in India.
A detailed chest scan revealed a large infected area in the lung, suggesting a long-standing problem. The procedure to closely evaluate the lungs was performed at the Yashoda Institute of Respiratory Medicine and Interventional Pulmonology, under the care of Dr. Ankit Bhatia and Dr. Rajesh Gupta. During the procedure, the patient developed a temporary complication, which was promptly managed, and he recovered well.
Further tests confirmed a rare fungal infection - Aspergillus Niger of the lung. Once the correct diagnosis was established, the patient was started on appropriate treatment and showed steady improvement.
Follow-up scans later confirmed complete healing of the lung. The patient has since returned in good health and expressed his heartfelt appreciation to the medical team.
The case highlights the importance of timely diagnosis, focused treatment, and experienced medical care in managing complex lung infections, and reflects the growing role of Indian medical institutions in treating patients from across the world.
Treatment By:
Dr. Ankit Bhatia and Dr. Rajesh Gupta

A 28-year-old male from Nepal was diagnosed with chronic kidney disease after experiencing persistent weakness and loss of appetite for nearly two years. Investigations revealed severely impaired kidney function, and he was initiated on hemodialysis through a catheter placed in the right side of his neck. He was advised to undergo AV fistula creation and maintain regular maintenance hemodialysis (MHD) three times a week.
However, due to irregular dialysis sessions, his condition worsened. He then consulted the expert team of nephrologists, Dr. Prajit Mazumdar and Dr. Inderjit G. Momin, along with urologists, Dr. Vaibhav Sax...
A 28-year-old male from Nepal was diagnosed with chronic kidney disease after experiencing persistent weakness and loss of appetite for nearly two years. Investigations revealed severely impaired kidney function, and he was initiated on hemodialysis through a catheter placed in the right side of his neck. He was advised to undergo AV fistula creation and maintain regular maintenance hemodialysis (MHD) three times a week.
However, due to irregular dialysis sessions, his condition worsened. He then consulted the expert team of nephrologists, Dr. Prajit Mazumdar and Dr. Inderjit G. Momin, along with urologists, Dr. Vaibhav Saxena and Dr. Kuldeep Agarwal, at Yashoda Medicity. The team counselled him regarding renal replacement therapy (RRT), the importance of regular MHD, and recommended renal transplantation as the most effective long-term solution.
His transplant evaluation began with his mother as the donor. During the assessment, he was found to have significant anaemia and reduced cardiac function, likely resulting from inconsistent dialysis, which increased his peri-operative risk. After thorough counselling, he was optimised for surgery, and immunosuppressive therapy was initiated two days prior to the procedure.
The patient successfully underwent renal transplantation with ATG induction. Post-surgery, he showed excellent recovery with good urine output and steadily improving creatinine levels. He was discharged with a creatinine of 1.2 mg/dl and continues to do well on follow-up.
Treatment By:
Dr. Vaibhav Saxena, Dr. Kuldeep Agarwal, Dr. Prajit Mazumdar, and Dr. Inderjit G. Momin

Conquering a Complex Brain Aneurysm with Advanced Endovascular Therapy
A patient with a spinal condition was treated at Yashoda Medicity through a navigation-guided minimally invasive spine surgery, marking the first such procedure in the state. The surgery was performed in our state-of-the-art Neuro-Spine OT, equipped with O-arm, Stealth-8 Neuronavigation, Allen table, and IONM.
The procedure was led by Dr. Dibya Jyoti Mahakul, Consultant – Minimally Invasive Neuro-Spine Surgeon, who performed the surgery with unmatched precision. Using the neuronavigation system, the team could visualize the move...
Conquering a Complex Brain Aneurysm with Advanced Endovascular Therapy
A patient with a spinal condition was treated at Yashoda Medicity through a navigation-guided minimally invasive spine surgery, marking the first such procedure in the state. The surgery was performed in our state-of-the-art Neuro-Spine OT, equipped with O-arm, Stealth-8 Neuronavigation, Allen table, and IONM.
The procedure was led by Dr. Dibya Jyoti Mahakul, Consultant – Minimally Invasive Neuro-Spine Surgeon, who performed the surgery with unmatched precision. Using the neuronavigation system, the team could visualize the movements of all instruments in real time, ensuring the accurate placement of implants.
The minimally invasive approach resulted in minimal blood loss and muscle damage, and the patient experienced immediate pain relief. This achievement underscores our commitment to leveraging cutting-edge technology to provide safe, precise, and effective surgical solutions for spine problems.
At Yashoda Medicity, we care about your back. When it comes to spine conditions, you’re in safe hands.
Treatment By:
Dr. Dibya Jyoti Mahakul
First Navigation-Guided Minimally Invasive Spine Surgery at Yashoda Medicity
A patient with a spinal condition was treated at Yashoda Medicity through a navigation-guided minimally invasive spine surgery, marking the first such procedure in the state. The surgery was performed in our state-of-the-art Neuro-Spine OT, equipped with O-arm, Stealth-8 Neuronavigation, Allen table, and IONM.
The procedure was led by Dr. Dibya Jyoti Mahakul, Consultant – Minimally Invasive Neuro-Spine Surgeon, who performed the surgery with unmatched precision. Using the neuronavigation system, the team could visualize the mo...
First Navigation-Guided Minimally Invasive Spine Surgery at Yashoda Medicity
A patient with a spinal condition was treated at Yashoda Medicity through a navigation-guided minimally invasive spine surgery, marking the first such procedure in the state. The surgery was performed in our state-of-the-art Neuro-Spine OT, equipped with O-arm, Stealth-8 Neuronavigation, Allen table, and IONM.
The procedure was led by Dr. Dibya Jyoti Mahakul, Consultant – Minimally Invasive Neuro-Spine Surgeon, who performed the surgery with unmatched precision. Using the neuronavigation system, the team could visualize the movements of all instruments in real time, ensuring the accurate placement of implants.
The minimally invasive approach resulted in minimal blood loss and muscle damage, and the patient experienced immediate pain relief. This achievement underscores our commitment to leveraging cutting-edge technology to provide safe, precise, and effective surgical solutions for spine problems.
At Yashoda Medicity, we care about your back. When it comes to spine conditions, you’re in safe hands.
Treatment By:
Dr. Dibya Jyoti Mahakul
First Awake Brain Surgery at Yashoda Medicity
At Yashoda Medicity, we don’t just operate on brain tumors – we preserve normal brain functions too. We successfully performed our first awake brain surgery in our state-of-the-art Neurosurgery OT, equipped with the Kinevo 900 operating microscope with 3D exoscope, fluorescence filters, Stealth-8 neuronavigation system, BK 5000 intraoperative ultrasound, IONM, and CUSA.
Led by Dr. Dibya Jyoti Mahakul, Consultant - Minimal invasive Brain, Spine and Endovascular Neurosurgery and supported by our expert neuroanaesthesia team and neuropsychologist, the p...
First Awake Brain Surgery at Yashoda Medicity
At Yashoda Medicity, we don’t just operate on brain tumors – we preserve normal brain functions too. We successfully performed our first awake brain surgery in our state-of-the-art Neurosurgery OT, equipped with the Kinevo 900 operating microscope with 3D exoscope, fluorescence filters, Stealth-8 neuronavigation system, BK 5000 intraoperative ultrasound, IONM, and CUSA.
Led by Dr. Dibya Jyoti Mahakul, Consultant - Minimal invasive Brain, Spine and Endovascular Neurosurgery and supported by our expert neuroanaesthesia team and neuropsychologist, the patient was kept awake during key parts of the procedure, allowing continuous monitoring of neurological function.
This milestone underscores our commitment to precision-driven, comprehensive care for patients with brain tumors. It reflects our dedication to bringing cutting-edge technology to society and providing safer neurosurgical options, resulting in faster recovery and better outcomes.
When it comes to brain surgeries, you’re in expert hands at Yashoda Medicity.
Treatment By:
Dr. Dibya Jyoti Mahakul
A 4-year-old, 11 kg child was brought to the Department of Pediatric Cardiac Sciences at Yashoda Medicity, Indirapuram, with complaints of bluish discoloration of fingernails and toes, poor weight gain, easy fatigue on walking, and recurrent hospital admissions.
Clinical evaluation revealed an oxygen saturation of 75%, prompting further investigations including echocardiography and CT pulmonary angiography.
The child was diagnosed with Cyanotic Congenital Heart Disease known as Tetralogy of Fallot (TOF), with additional apical muscular VSD and a hypoplastic pulmonary annulus.
The patient underwent open-heart surg...
A 4-year-old, 11 kg child was brought to the Department of Pediatric Cardiac Sciences at Yashoda Medicity, Indirapuram, with complaints of bluish discoloration of fingernails and toes, poor weight gain, easy fatigue on walking, and recurrent hospital admissions.
Clinical evaluation revealed an oxygen saturation of 75%, prompting further investigations including echocardiography and CT pulmonary angiography.
The child was diagnosed with Cyanotic Congenital Heart Disease known as Tetralogy of Fallot (TOF), with additional apical muscular VSD and a hypoplastic pulmonary annulus.
The patient underwent open-heart surgery called Intracardiac Repair, including closure of multiple VSDs with a transannular patch over the neopulmonary valve. The procedure was led by Dr. Abhinavsingh Chauhan, Consultant Pediatric Cardio-thoracic and Vascular Surgery. Advanced post-operative care in the Pediatric Cardiac ICU was uneventful, and post-operative echocardiography confirmed a successful repair.
The child was discharged in a stable and ambulatory condition on the 5th post-operative day, with oxygen saturation improving to 99%. This case reflects Yashoda Medicity’s expertise in managing complex pediatric cardiac conditions, combining cutting-edge surgical techniques with specialized intensive care to ensure safe, life-transforming outcomes for children.
Treatment By:
Dr. Abhinavsingh Chauhan
An International patient from Myanmar with Mitral Regurgitation, pulmonary hypertension and low ejection fraction-35% underwent successful transplant
A middle aged male was diagnosed with chronic kidney disease when he developed generalized body weakness, puffiness of face and swelling of legs with nausea, intermittent vomiting . On Investigations, he was found to have deranged renal function with urea-300 mg/dl,creatinine of 15 mg/dl, hb-9 mg and was subsequently started on hemodialysis via catheter inserted in right side of neck.
He subsequently visited India where he consulted our expert tea...
An International patient from Myanmar with Mitral Regurgitation, pulmonary hypertension and low ejection fraction-35% underwent successful transplant
A middle aged male was diagnosed with chronic kidney disease when he developed generalized body weakness, puffiness of face and swelling of legs with nausea, intermittent vomiting . On Investigations, he was found to have deranged renal function with urea-300 mg/dl,creatinine of 15 mg/dl, hb-9 mg and was subsequently started on hemodialysis via catheter inserted in right side of neck.
He subsequently visited India where he consulted our expert team of doctors-Dr Prajit Mazumdar, Dr Inderjit G Momin,Dr Vaibhav Saxena and Dr Kuldeep Agarwal at Yashoda superspeciality Hospital, Kausambi who advised her to under renal transplant as it is the best form of renal replacement therapy. His Transplant workup was subsequently started and donor was wife and blood group was same.
However on transplant work up, it was found that he had Mitral Regurgitation, pulmonary hypertension and low ejection fraction-35% which increased his peri operative risk. Subsequently he was started on medicines and decongestion was done with diuretics and intensive hemodialysis. Subsequently renal transplantation was done after obtaining cardiology clearance with moderate risk and explaining the risk.
He underwent renal transplantation with Solumedrol and ATG induction. After transplantation he had good urine output with decreasing creatinine and was subsequently discharged with creatinine of 1.2 mg/dl . After transplant his pulmonary hypertension decreased and mitral regurgitation decreased which proves renal replacement therapy in form of transplant leads to improvement of cardiac condition. He is doing well on OPD follow up even today, 1.5 year after transplant with stable graft function and enjoying his life in myanmar.
Treatment By:
Dr Prajit Mazumdar, Dr Inderjit G. Momin, Dr Vaibhav Saxena, and Dr Kuldeep Agarwal
A challenging case of Erythroderma in a young male patient.
A 31-year-old male presented to our dermatology OPD with severe redness and flakiness of skin all over the body. The symptoms had been present for two months, with a marked worsening in the last 15 days. After a detailed history, examination, and workup, the patient was diagnosed with Erythroderma – a serious condition where there is erythema and scaling over more than 90% of the body surface area. Despite having experienced similar skin problems in the past, the patient had never received a correct diagnosis and was unaware of the underlying dis...
A challenging case of Erythroderma in a young male patient.
A 31-year-old male presented to our dermatology OPD with severe redness and flakiness of skin all over the body. The symptoms had been present for two months, with a marked worsening in the last 15 days. After a detailed history, examination, and workup, the patient was diagnosed with Erythroderma – a serious condition where there is erythema and scaling over more than 90% of the body surface area. Despite having experienced similar skin problems in the past, the patient had never received a correct diagnosis and was unaware of the underlying disorder that could have led to Erythroderma.
Given the extensive nature of skin involvement and risk of serious complications, he was admitted for detailed evaluation and prompt management. A thorough workup was performed, and appropriate medical treatment was initiated. Over the course of 7–10 days, the patient showed remarkable clinical improvement; the skin lesions resolved significantly, systemic parameters stabilized, and he was safely discharged.
Most importantly, after nearly 3–4 years of recurrent but undiagnosed skin issues, the patient was finally diagnosed with atopic dermatitis. This accurate diagnosis not only explained his longstanding symptoms but also enabled the initiation of targeted treatment and counseling regarding long-term care and preventive measures. With this approach, the patient was able to move beyond temporary symptom relief toward effective disease control and an improved quality of life.
Treatment By:
Dr. Kriti Maheshwari

A 4-year-old male child with congenital Pelvi-Ureteric Junction (PUJ) Obstruction underwent Robot-Assisted Pyeloplasty at Yashoda Medicity. The child had an excellent postoperative recovery and was discharged on postoperative day 2.
Robotic surgery offers superior precision and control, providing a significant advantage not only in cancer surgeries but also in pediatric minimally invasive procedures.
The benefits of robotic surgery over conventional techniques include smaller incisions, minimal intraoperative blood loss, enhanced surgical precision and dissection, reduced postoperative pain, and faster recovery and di...
A 4-year-old male child with congenital Pelvi-Ureteric Junction (PUJ) Obstruction underwent Robot-Assisted Pyeloplasty at Yashoda Medicity. The child had an excellent postoperative recovery and was discharged on postoperative day 2.
Robotic surgery offers superior precision and control, providing a significant advantage not only in cancer surgeries but also in pediatric minimally invasive procedures.
The benefits of robotic surgery over conventional techniques include smaller incisions, minimal intraoperative blood loss, enhanced surgical precision and dissection, reduced postoperative pain, and faster recovery and discharge.
The Department of Urology at Yashoda Medicity is committed to providing the highest standard of care to every patient, with special expertise in Robotic Surgery, Reconstructive Urology, Uro-Oncology, Stone Diseases, and Renal Transplant Surgeries.
Treatment By:
Dr. Vaibhav Saxena
The Department of Urology at Yashoda Medicity, Indirapuram, headed by Dr. Vaibhav Saxena, a pioneer in Robotic Urological Surgeries, has successfully performed a wide range of robotic procedures in both Urology and Uro-Oncology. Patients from across India have been successfully treated for various cancers and other urological conditions.
Among his recent notable cases was a Robotic Radical Cystectomy with Pelvic Lymph Node Dissection and Intracorporeal Urinary Diversion, performed on a patient who had travelled from Mathura for treatment. The patient had previously received neoadjuvant chemoradiation but developed a recurre...
The Department of Urology at Yashoda Medicity, Indirapuram, headed by Dr. Vaibhav Saxena, a pioneer in Robotic Urological Surgeries, has successfully performed a wide range of robotic procedures in both Urology and Uro-Oncology. Patients from across India have been successfully treated for various cancers and other urological conditions.
Among his recent notable cases was a Robotic Radical Cystectomy with Pelvic Lymph Node Dissection and Intracorporeal Urinary Diversion, performed on a patient who had travelled from Mathura for treatment. The patient had previously received neoadjuvant chemoradiation but developed a recurrence in the urinary bladder. Curative robotic surgery was deemed the best option. The patient underwent a successful procedure and was discharged on the fifth postoperative day.
Treatment By:
Dr. Vaibhav Saxena
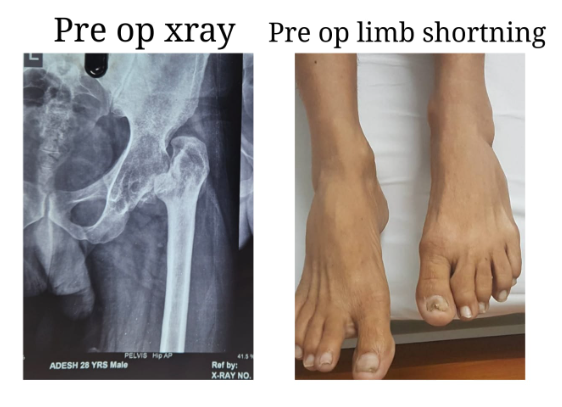
Total Hip Replacement in a Young Adult with Secondary Osteoarthritis of the Hip due to Sequelae of Childhood Septic Arthritis
Early and effective treatment of childhood hip septic arthritis is crucial to prevent or minimize long-term complications such as avascular necrosis, hip dislocation, osteoarthritis, and leg length discrepancy.
We present a case of a 30-year-old male patient suffering from secondary osteoarthritis of the left hip, with complete destruction of the joint over the past 20 years. He had septic arthritis of the left hip at the age of 9, which was only partially treated, resulting i...
Total Hip Replacement in a Young Adult with Secondary Osteoarthritis of the Hip due to Sequelae of Childhood Septic Arthritis
Early and effective treatment of childhood hip septic arthritis is crucial to prevent or minimize long-term complications such as avascular necrosis, hip dislocation, osteoarthritis, and leg length discrepancy.
We present a case of a 30-year-old male patient suffering from secondary osteoarthritis of the left hip, with complete destruction of the joint over the past 20 years. He had septic arthritis of the left hip at the age of 9, which was only partially treated, resulting in long-term sequelae.
This was a challenging case due to the chronic arthritic hip and associated soft tissue contractures. We performed an uncemented total hip replacement with subtrochanteric osteotomy. The procedure proceeded as planned: the limb length discrepancy was corrected, and the patient was mobilized within 24 hours. He was discharged after four days, pain-free, and walking with support.
He is expected to achieve full weight-bearing and return to all activities of daily living within eight to ten weeks.
Treatment By:
Dr. Amit Sharma

A new life donated to daughter-in law by mother in law
A 30-year-old female was diagnosed with chronic kidney disease after presenting with generalised weakness, loss of appetite, and intermittent vomiting. Investigations revealed impaired renal function, and she was started on haemodialysis through a catheter placed in the right side of her neck. She was advised maintenance haemodialysis three times a week.
She consulted our expert team of doctors including Dr Prajit Mazumdar, Dr Inderjit G. Momin, Dr Vaibhav Saxena, and Dr Kuldeep Agarwal at Yashoda Superspeciality Hospital, Kaushambi. They recomme...
A new life donated to daughter-in law by mother in law
A 30-year-old female was diagnosed with chronic kidney disease after presenting with generalised weakness, loss of appetite, and intermittent vomiting. Investigations revealed impaired renal function, and she was started on haemodialysis through a catheter placed in the right side of her neck. She was advised maintenance haemodialysis three times a week.
She consulted our expert team of doctors including Dr Prajit Mazumdar, Dr Inderjit G. Momin, Dr Vaibhav Saxena, and Dr Kuldeep Agarwal at Yashoda Superspeciality Hospital, Kaushambi. They recommended renal transplantation as the most effective form of renal replacement therapy. Her transplant workup was initiated, with her mother considered as the first donor option.
However, her mother was found to have diabetes, her father had a cardiac condition, and her husband was not a compatible blood group. With limited donor options, her mother-in-law, who had a matching blood group, came forward to donate a kidney and save her daughter-in-law’s life.
After obtaining clearance from cardiology, pulmonology, gynaecology, and psychiatry, along with approval from the authorisation committee, the transplant was successfully carried out with ATG induction. Post-transplant, she maintained good urine output with steadily improving creatinine levels. She was discharged with a creatinine of 1.2 mg/dl. The donor also recovered well and continues to do fine.
Treatment By:
Dr Prajit Mazumdar, Dr Inderjit G. Momin, Dr Vaibhav Saxena, and Dr Kuldeep Agarwal
An International patient from Myanmar with Mitral Regurgitation, pulmonary hypertension, and low ejection fraction-35% underwent successful transplant
A middle-aged male was diagnosed with chronic kidney disease after developing generalised weakness, facial puffiness, swelling of the legs, nausea, and intermittent vomiting. Investigations revealed severely impaired renal function with urea of 300 mg/dl, creatinine of 15 mg/dl, and haemoglobin of 9 g/dl. He was started on haemodialysis through a catheter placed in the right side of his neck.
He later visited India and consulted our expert team of doct...
An International patient from Myanmar with Mitral Regurgitation, pulmonary hypertension, and low ejection fraction-35% underwent successful transplant
A middle-aged male was diagnosed with chronic kidney disease after developing generalised weakness, facial puffiness, swelling of the legs, nausea, and intermittent vomiting. Investigations revealed severely impaired renal function with urea of 300 mg/dl, creatinine of 15 mg/dl, and haemoglobin of 9 g/dl. He was started on haemodialysis through a catheter placed in the right side of his neck.
He later visited India and consulted our expert team of doctors, including Dr Prajit Mazumdar, Dr Inderjit G. Momin, Dr Vaibhav Saxena, and Dr Kuldeep Agarwal at Yashoda Superspeciality Hospital, Kaushambi. Renal transplantation was advised as the most effective form of renal replacement therapy. His transplant workup was initiated, and his wife, who had a matching blood group, volunteered to donate.
During the evaluation, he was found to have mitral regurgitation, pulmonary hypertension, and a reduced ejection fraction of 35 percent, which significantly increased his perioperative risk. He was started on medications, optimised with diuretics, and maintained on intensive haemodialysis for decongestion. After cardiology clearance and counselling regarding moderate surgical risk, renal transplantation was planned.
He successfully underwent renal transplantation with Solumedrol and ATG induction. Post-transplant, he maintained good urine output with steadily decreasing creatinine levels and was discharged with a creatinine of 1.2 mg/dl. His pulmonary hypertension and mitral regurgitation also improved, demonstrating the positive impact of renal transplantation on cardiac function.
He continues to do well on outpatient follow-up, one and a half years after transplant, with stable graft function, and is enjoying a healthy life in Myanmar.
Treatment By:
Dr Prajit Mazumdar, Dr Inderjit G. Momin, Dr Vaibhav Saxena, and Dr Kuldeep Agarwal

A case of ABO incompatible transplant with high ANTI B TITRES
A 37-year-old male was diagnosed with chronic kidney disease three years ago after presenting with frothy urine and hypertension. Initial investigations revealed a serum creatinine of 3 mg/dl. Over the next few years, his kidney function deteriorated, and he was started on maintenance haemodialysis three times a week via an arteriovenous fistula. He was referred to our hospital by a former recipient who had undergone renal transplantation under Dr Prajit Mazumdar. On evaluation by our team of doctors, the need for renal transplantation was expla...
A case of ABO incompatible transplant with high ANTI B TITRES
A 37-year-old male was diagnosed with chronic kidney disease three years ago after presenting with frothy urine and hypertension. Initial investigations revealed a serum creatinine of 3 mg/dl. Over the next few years, his kidney function deteriorated, and he was started on maintenance haemodialysis three times a week via an arteriovenous fistula. He was referred to our hospital by a former recipient who had undergone renal transplantation under Dr Prajit Mazumdar. On evaluation by our team of doctors, the need for renal transplantation was explained in view of end-stage renal disease.
His transplant workup was initiated, with his father considered as the first donor. However, he was rejected due to diabetes. Donor evaluation of his mother was then undertaken, but her blood group was incompatible with the recipient. In view of ABO incompatibility, anti-A and anti-B titres were assessed and revealed a high anti-B titre.
After detailed counselling regarding prognosis, risks, and cost, the family opted to proceed with an ABO-incompatible renal transplant. Rituximab was administered two weeks prior to transplantation, and he was started on tacrolimus and mycophenolate mofetil. This was followed by two sessions of Glycosorb column treatment on days 12 and 14, after which his anti-B titre decreased to 1:2. He then underwent renal transplantation with Solumedrol and Simulect induction, with anti-B titres monitored every 12 hours.
Post-transplant, he maintained brisk urine output and his serum creatinine gradually declined. He was discharged with a creatinine of 1.2 mg/dl and continues to do well on follow-up.
Treatment By:
Dr Prajit Mazumdar
A challenging Case of renal transplant with a history of >22 units of blood transfusion and class 1 DSA positive
A 26-year-old male was diagnosed with chronic kidney disease after developing generalised weakness and loss of appetite. Investigations revealed impaired renal function with a creatinine of 12 mg/dl and haemoglobin of 5 g/dl. He was started on haemodialysis through a catheter placed in the right side of his neck and advised AV fistula creation with maintenance haemodialysis three times a week.
Despite regular dialysis, his anaemia persisted and he required multiple blood transfusions (more...
A challenging Case of renal transplant with a history of >22 units of blood transfusion and class 1 DSA positive
A 26-year-old male was diagnosed with chronic kidney disease after developing generalised weakness and loss of appetite. Investigations revealed impaired renal function with a creatinine of 12 mg/dl and haemoglobin of 5 g/dl. He was started on haemodialysis through a catheter placed in the right side of his neck and advised AV fistula creation with maintenance haemodialysis three times a week.
Despite regular dialysis, his anaemia persisted and he required multiple blood transfusions (more than 22 units over three months) even while receiving erythropoietin and iron therapy. Anaemia workup revealed occult blood in the stool, and upper GI endoscopy confirmed peptic ulcer disease.
He consulted our team of nephrologists (Dr Prajit Mazumdar and Dr Inderjit G. Momin) and urologists (Dr Vaibhav Saxena and Dr Kuldeep Agarwal) at Yashoda Superspeciality Hospitals, Kaushambi, where renal transplantation was advised. His mother, who had a matching blood group, was identified as the donor. However, transplant workup revealed donor-specific antibodies on single antigen bead testing (Class I) with an MFI greater than 2500 on multiple beads, most likely due to the multiple blood transfusions. This significantly increased the risk of acute rejection in the immediate post-transplant period, making the case high-risk.
After thorough counselling regarding risks, he underwent desensitisation with two sessions of plasmapheresis and IVIg to reduce the donor-specific antibodies. He then successfully underwent renal transplantation with ATG induction. Post-transplant, he maintained good urine output with steadily improving creatinine levels and was discharged with a creatinine of 1.2 mg/dl.
He continues to do well on outpatient follow-up.
Treatment By:
Dr Prajit Mazumdar, Dr Inderjit G. Momin, Dr Vaibhav Saxena, and Dr Kuldeep Agarwal

Conquering a Complex Brain Aneurysm with Advanced Endovascular Therapy
Brain aneurysms are often described as ticking time bombs—silent, unpredictable, and potentially life-threatening if left untreated. They pose one of the most complex challenges in modern neurosurgery, requiring both precision and cutting-edge technology for successful management.
A 60-year-old woman presented with multiple episodes of severe headache, prompting her to consult Dr. Sumantao Chaterjee (Neurologist). Given the persistence and pattern of her symptoms, a brain angiography was recommended and performed by Dr. ...
Conquering a Complex Brain Aneurysm with Advanced Endovascular Therapy
Brain aneurysms are often described as ticking time bombs—silent, unpredictable, and potentially life-threatening if left untreated. They pose one of the most complex challenges in modern neurosurgery, requiring both precision and cutting-edge technology for successful management.
A 60-year-old woman presented with multiple episodes of severe headache, prompting her to consult Dr. Sumantao Chaterjee (Neurologist). Given the persistence and pattern of her symptoms, a brain angiography was recommended and performed by Dr. Dibya Jyoti Mahakul (Endovascular Neurosurgeon).
The imaging revealed a complex brain aneurysm, one that demanded meticulous planning due to its size, shape, location, and blood flow dynamics. After careful evaluation, the patient was offered a scarless, minimally invasive endovascular treatment. A flow diverter stent was strategically placed across the neck of the aneurysm to divert blood flow away from the aneurysm sac, promoting healing and preventing rupture. While technically challenging, the procedure was greatly aided by our state-of-the-art biplanar cath lab, equipped with advanced imaging tools like Vaso CT, CBCT, and MAFA software. These technologies ensured maximum precision, safety, and speed for both the patient and surgical team. Remarkably, the patient was discharged the very next day in a stable condition—aneurysm secured, risk averted.
Today, she is back home with her family, free from the shadow of a life-threatening condition, and ready to embrace life on her own terms.
Treatment By:
Dr. Dibya Jyoti Mahakul, Dr. Sumantao Chaterjee

A 51-year-old lady with left arm pain more than neck pain of 10 years duration, with BMI 44 and a short neck nearly the chin touching the chest, was diagnosed with OPLL C3-6 with myelopathy and fixed kyphosis of 20°. MRI showed cord signal changes at C5, and CT confirmed OPLL C3 -6 with high probability of intradural mass ( double density sign). Conventional wisdom (K line, kyphosis, anterior pathology etc.) dictated towards an anterior surgery, but possibility of dural laceration (intradural OPLL mass), with potential for other complications (cord / trachea / esophageal compression by pseudomeningole, meningitis, spinal cord ...
A 51-year-old lady with left arm pain more than neck pain of 10 years duration, with BMI 44 and a short neck nearly the chin touching the chest, was diagnosed with OPLL C3-6 with myelopathy and fixed kyphosis of 20°. MRI showed cord signal changes at C5, and CT confirmed OPLL C3 -6 with high probability of intradural mass ( double density sign). Conventional wisdom (K line, kyphosis, anterior pathology etc.) dictated towards an anterior surgery, but possibility of dural laceration (intradural OPLL mass), with potential for other complications (cord / trachea / esophageal compression by pseudomeningole, meningitis, spinal cord hernia etc.) were discussed in detail and a decission was taken to decompress and fix from the posterior aspect. The pre-op CT angio showed B/L high-riding vertebral arteries, which precluded the C2 screw.
Per operatively, the patient was positioned prone with the head clamped and a posterior exposure done. LM screw entry points were made from C3-6, followed by grade 1 facet resection at C3-4, C4-5, and C5-6 bilaterally. Further lordosis was achieved with manipulation of the head with the head clamp and closing the osteotomy gaps. LM screws (C3-6), a laminar screw at C2, and a pedicle screw at T1 & 2 were inserted and connected with rods.
C3-6 laminectomy was done, and the surgical site was closed after bone graft mixed with vancomycin was applied laterally.
Postoperative x-ray showed adequate lordosis (approximately 10 degrees) attainment.
The patient reported complete pain relief in the left shoulder and arm postoperatively.
Treatment By:
Dr. Ankur Goswami

A tremendous job has been done by Dr. Amit Sharma. I met with an accident in which the ACL ligament of my left knee was completely torn. I met Dr. Amit Sharma then he analysed the situation and told us about the procedure and the time period to recover from the injury. He has performed a successful surgery. The good thing is the confidence that Dr. Amit Sharma has on his surgery that he didn’t put braces on the knee while other doctors put the braces on for a month and then started Physiotherapy which will take a longer time period to heal from the injury.
Dr. Amit Sharma has started the Physiotherapy from the very next day of the surgery and i was discharged in 2 days, and the Physiotherapy is undergoing at my home. It's the 10th day today and I have gained so much confidence in 10 days that I am recovering very fast and in a few weeks I will be able to walk without any support.
Thanks to Dr. Amit Sharma, he is really having magical hands, he is very kind in nature, in my regular visits all of my stress went away after talking to him.
Again Thank You so much Doctor
Treatment By:
Dr. Amit Sharma
Beyond Doubt, THE BEST GYNAECOLOGIST IN DELHI/NCR and by far margin. She has tremendous knowledge in her field. Listens very carefully and patiently to all the problems and provides advice and solutions accordingly. Tough cases become ridiculously easy for her and she solves all the problems of the patient with a very nice smile. My wife had some complications in her pregnancy but she had solved all the problems with ease and my wife had normal delivery. I had visited many hospitals including Motherhood and Cloudnine hospital. Dr. Sneha Mishra is the Best Maternity doctor in Noida and Ghaziabad.
We are blessed to have a babyboy last week with normal delivery process.
We want to express our heartfelt gratitude to our doctor Dr. Sneha Mishra for the exceptional care and support during labor and delivery. Your kindness and dedication made a significant impact on our journey. “We’re so glad to have had you in our corner during the birthing process. Thank you for being an amazing part of our special time.”
I highly recommend Dr. Sneha Mishra Ma’am. My wife conceived twin babies by the helpful hand of Dr. Sneha Mishra Ma’am. She is incredibly knowledgeable, practiced, and passionate about her work. She is friendly, caring, and accommodating. She is punctual and efficient, making my wife feel like her concerns were truly valued. “Dr. Sneha Mishra is a great doctor. She is very particular and gentle about mother & baby care.”
I recently underwent an IVF procedure at Yashoda Hospital, Karkarduma, under the expert guidance of Dr. Sneha Mishra, and I must say that my experience was truly exceptional. From the very beginning, the entire team was extremely supportive, caring, and professional. They provided ample time and guidance throughout the process, ensuring that we felt comfortable and well-informed at every step.
Dr. Sneha Mishra was outstanding—her expertise, patience, and compassionate approach made this journey much smoother for us. I am truly grateful for her dedication and care.
A special mention to Sunayna, the coordinator between the doctor and patients. She played a crucial role in seamless communication. Since my home is quite far from the hospital, she ensured that I received timely updates and responses over the phone, which made the entire process much more convenient. Her professionalism and prompt coordination deserve appreciation.
I was blessed with a baby boy 20 days back. The way Dr. Sneha handled my entire pregnancy and delivery was commendable. She never asked for unnecessary tests/scans. She was always available for all my queries. She definitely has a personal touch with her patients. She was always positive in her approach and helped me steer through pregnancy in a most convenient manner. Since it was my first pregnancy, I was extremely scared of delivery but Dr. Sneha made everything smooth and comfortable for me and I highly recommend her to all.
